Health Equity Research Network on Disparities in Maternal-Infant Health Outcomes
HERN Disparities in Maternal-Infant Health Outcomes
P3 EQUATE Awardee Teams
The AHA has committed $20 million to establish this Health Equity Research Network (HERN), which provides an opportunity to significantly advance our understanding of the factors underlying the disproportionate impact of maternal mortality and morbidity on Black women, Native American women, and those living in rural areas. Because heart and vascular issues account for about half of these deaths, the AHA is uniquely positioned to address this critical issue.
P3 (Pregnancy and Postpartum/Postnatal) EQUATE (Enhancing Access and QUAlity To Achieve Equitable Maternal and Infant Health)
The overriding goal of the P3 EQUATE Health Equity Research Network is to promote equity in Maternal and Infant Health outcomes by identifying innovative and cost-effective strategies to enhance access to quality health information, care, and experiences during preconception, pregnancy, and postpartum periods, particularly for Black and underserved populations. Our team will collaborate with pregnant and postpartum people and their families, hospitals, and communities to discover ways to reduce racism and social issues that contribute to poor health outcomes.
The network is managed by a team from the University of Alabama at Birmingham (UAB) led by Alan T. Tita, M.D., Ph.D., M.P.H., senior vice-chair for research and innovation in the Department of Obstetrics and Gynecology, associate dean for global and women’s health at the UAB Heersink School of Medicine, and the director of the Center for Women’s Reproductive Health at UAB.
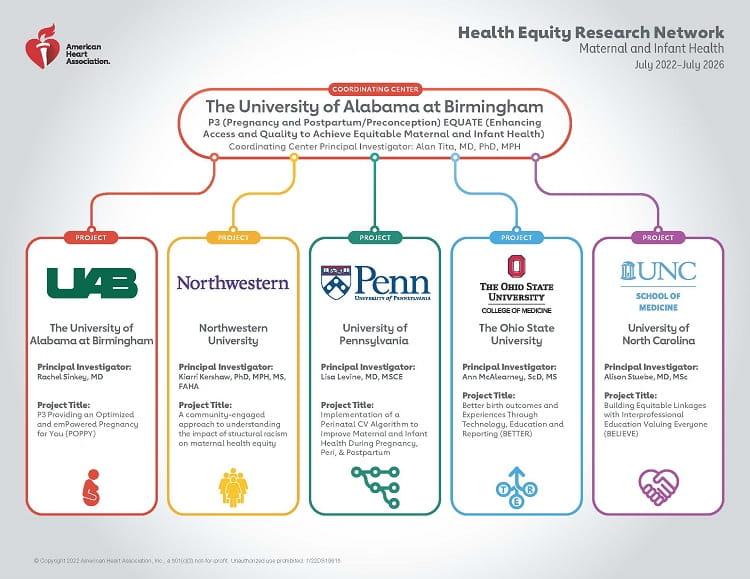
Five targeted research projects began on July 1, 2022, and will run for four years:
A community-engaged approach to understanding the impact of structural racism on maternal health equity at Northwestern University – led by Kiarri Kershaw, Ph.D., M.P.H., M.S., an associate professor of preventive medicine (epidemiology) at Northwestern’s Feinberg School of Medicine, this team will identify the best ways to address the negative impacts of structural racism on Black-white inequities in pregnancy outcomes and heart disease risk. The team will work with a diverse group of pregnant people from different areas, along with other community members and organizations to create a way to measure structural racism. Using data from pregnant participants in the study, the team will calculate the impact that addressing structural racism has on Black-white inequities in the health of parents and babies to find ways to reduce health inequities among pregnant people and infants.
Better birth outcomes and Experiences Through Technology, Education and Reporting (BETTER) at The Ohio State University (OSU) – led by Ann Scheck McAlearney, Sc.D., M.S., distinguished professor of family and community medicine, associate dean for health services research and executive director of CATALYST, the Center for the Advancement of Team Science, Analytics and Systems Thinking in Health Services and Implementation Science Research in the OSU College of Medicine, this team will design and test a new way to improve the health of pregnant people and their babies by targeting social problems that can increase risk, such as not having a place to live, not having enough food, or living with crime and violence. The team will work closely with pregnant people to learn from them about the problems they see as most important, and how they would like to communicate about those issues during their care. They will also talk to doctors and nurses to understand how clinicians would like to learn about these issues as they care for pregnant people. With this understanding, the team will develop, implement and test an intervention to determine whether and how learning about and addressing social problems for pregnant people can help improve the health of pregnant people and their babies.
P3 Providing an Optimized and emPowered Pregnancy for You (POPPY) at the University of Alabama at Birmingham – led by Rachel G. Sinkey, M.D., an assistant professor of obstetrics and gynecology and Wally Carlo, M.D., a professor of pediatrics at UAB, this team will study two ways to improve care for pregnant people and their babies: 1) a digital health intervention and 2) a community health worker intervention. The digital health intervention sends text messages to pregnant people with important health reminders and the expectant person can, in turn, ask questions through texting and get answers in real-time. The team will gain insight from participants about what they consider most important and helpful about the text messages to further refine the communications. In the second intervention, the community health workers check in on the pregnant people regularly, offering key health reminders every two weeks, helping with transportation and even accompanying them to doctors’ visits, if needed. Finally, the team will test to see if the texting and community health worker interventions lead to better outcomes.
Building Equitable Linkages with Interprofessional Education Valuing Everyone (BELIEVE) at the University of North Carolina at Chapel Hill (UNC-CH) in collaboration with North Carolina Agricultural and Technical State University (N.C. A&T)– led by Alison M. Stuebe, M.D., M.Sc., a maternal-fetal medicine subspecialist and professor of obstetrics and gynecology and Kimberly D. Harper, M.S.N., R.N., M.H.A., a registered nurse in maternal and child health both from UNC-CH and by Kimberly C. Harper, Ph.D, a professor of English and researcher in Black maternal health and ethos, Black rhetoric of healthcare and reproductive justice, and Janiya Mitnaul Williams, M.A., IBCLC, CLC, a lactation consultant and the program director of the Human Lactation Program both from N.C. A&T, this team will work with community and health team members to develop a training focused on healing the traumas experienced by families, pregnant people and health care team members as a result of structural determinants of health that are the root cause of health inequities in systems. The overall goal of the work is to transform health services so that each pregnant person and health care team member is seen, heard and valued. The team will use focus groups and web-based surveys to define equitable care and determine how to build trust in the health care system; use information from surveys and focus groups to create learning objectives and content to train medical students; and assess health outcomes after the training is implemented. The goal is to develop a training that can be used nationally to reduce disparities. The team hopes to find lower pain scores among Black people giving birth, less formula supplementation, more support for breastfeeding as appropriate and less negative comments in the medical chart once the training is in place.
Implementation and Evaluation of a Perinatal CV Risk-Assessment Algorithm to Improve Maternal and Infant Health During Pregnancy, Peri & Postpartum: IMPACT P3 at the University of Philadelphia - led by Lisa D. Levine, M.D., M.S.C.E., the Michael T. Mennuti, M.D., Associate Professor in Reproductive Health and Abike James, M.D., an associate professor of clinical obstetrics and gynecology at UPenn’s Perelman School of Medicine, this team will work to integrate into practice a cardiovascular (CV) risk-assessment for pregnant and postpartum patients that, if used correctly, could identify almost 90% of CV-related pregnancy deaths before they occur. The team will help medical providers ensure that patients get follow-up tests that are recommended through the assessment. They’ll put the assessment into practice, first in two hospitals in Philadelphia and then roll it out to all hospitals in Philadelphia to facilitate earlier diagnosis and treatment of pregnancy-related CVD. The team will track implementation outcomes, clinical outcomes, quality metrics and neonatal outcomes as an evaluation of effectiveness of this standardized CV risk. assessment.
Background
American Heart Association health equity research network will focus on identifying causes and finding solutions to improve outcomes among people who are more likely to experience pregnancy complications due to poor heart health
 More than one in four pregnancy-related deaths (26.5%) in the U.S. are tied to poor heart health, especially among people of color, putting both parents-to-be and their babies at risk, according to the American Heart Association Heart (AHA) Disease and Stroke Statistics 2022 Update. To address this issue, the AHA is funding a $20 million initiative comprised of a network of special projects focused on advancing the understanding of the factors underlying the disproportionate impact of pregnancy complications and deaths among Black and Native American pregnant people and those living in rural areas.
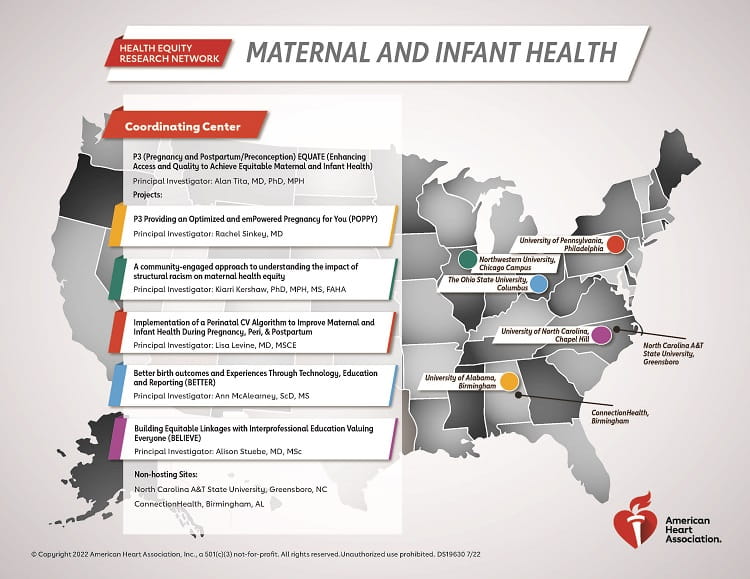
More than one in four pregnancy-related deaths (26.5%) in the U.S. are tied to poor heart health, especially among people of color, putting both parents-to-be and their babies at risk, according to the American Heart Association Heart (AHA) Disease and Stroke Statistics 2022 Update. To address this issue, the AHA is funding a $20 million initiative comprised of a network of special projects focused on advancing the understanding of the factors underlying the disproportionate impact of pregnancy complications and deaths among Black and Native American pregnant people and those living in rural areas.The Health Equity Research Network (HERN) on Disparities in Maternal-Infant Health Outcomes is part of the multi-pronged approach of the American Heart Association’s unprecedented pledge to aggressively address social determinants of health while working to improve health equity for all communities. Teams of scientists from North Carolina Agricultural and Technical State University in Greensboro (a Historically Black College and University/HBCU), Northwestern University in Chicago, The Ohio State University in Columbus, the University of Alabama at Birmingham, the University of North Carolina at Chapel Hill and University of Pennsylvania in Philadelphia will lead the community-engaged research projects. A team from the Center for Women’s Reproductive Health at the University of Alabama at Birmingham will serve as the coordinating center for the network, leveraging expertise across network sites and nationally, to help train the next generation of pregnancy health equity researchers, providing consultation and guidance, compiling data reports and coordinating the administration of the initiative.
Link to AHA Newsroom for announcement of the awardees.
Health Equity Research Network on Disparities in Maternal-Infant Health Outcomes (PDF)
Contact Us
General Questions:
[email protected]
Technical Support:
[email protected]
1-800-875-2562 (toll-free U.S. and Canada)
1-703-964-5840 (direct dial international)