Recurrent Pericarditis for Professionals
Recurrent Pericarditis
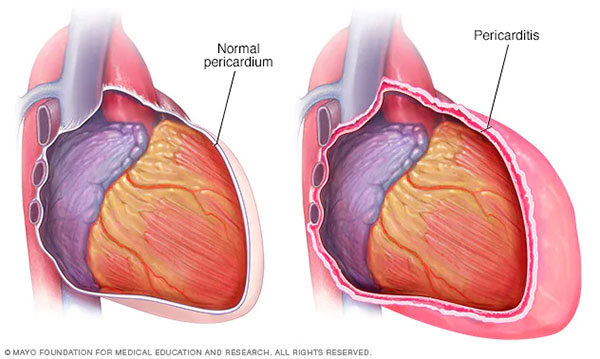
Recurrent pericarditis is a common complication after the first episode of pericarditis, characterized by the recurrence of chest pain and signs of cardiovascular inflammation. Recurrent pericarditis presents major short-term and long-term challenges for clinicians and patients alike.
The impact of recurrent pericarditis often extends beyond cardiac effects, with general uncertainty of each recurrence triggering anxiety, depression, and disruption in overall quality of life.
Recurrent Pericarditis: A Toolkit for Health Care Professionals

OnDemand Videos

Recurrent Pericarditis: Practical and Surgical Management
This expert-led video covers recurrent pericarditis management, emphasizing IL-1’s role in inflammation and recurrence, treatment strategies—including cardiac surgery—and a patient’s journey.
Acute Pericarditis: A Practical Approach to Diagnostic Evaluation & Initial Management
Enhance your understanding and skills in diagnosing and managing acute pericarditis with our on-demand video, available for healthcare professionals.
Special Topics in Recurrent Pericarditis: Recognize and Manage Refractory Disease
This webinar will explore the features of monogenic autoinflammatory diseases as a paradigm for IL-1 mediated recurrent pericarditis.
Acute Pericarditis: Recognition, Initial Management, and Preventing Recurrence
This webinar reviews pericarditis diagnosis, risk stratification, treatment strategies, and practical pharmacology for management and recurrence prevention.
Recurrent Pericarditis: Epidemiology, Presentation, Pathophysiology, and Diagnostic Testing
This webinar provides key takeaways for initial diagnosis and clinical evaluation strategies in recurrent pericarditis.HeartBEATS from Lifelong Learning™
Navigating Recurrent Pericarditis: Shared Decision Making and Patient Stories
Conventional Approaches to Managing Recurrent Pericarditis
IL-1 Blockade – Rationale, Evidence Base, and Practical Clinical Pharmacology
This vodcast helps healthcare professionals understand current guidelines, science, and best practices for managing recurrent pericarditis, focusing on IL-1 blockade, supporting evidence, and clinical pharmacology to improve patient outcomes.
Clinical Evaluation and Diagnostic Assessment
Management and Pharmacological Strategies
In this episode, experts discuss the initial pharmacologic management of acute pericarditis, offering practical insights to enhance your clinical skills.
Podcasts
Long Term Complications of Recurrent Pericarditis
Recurrent Pericarditis in Systemic Autoinflammatory and Autoimmune Disease – Clinical Recognition and Management
Recurrent Pericarditis: The Role of IL-1 Blockade
Pathophysiology of Recurrent Pericarditis
Beyond Acute – Recurrent Pericarditis
Treatment of Acute Pericarditis
Complications of Acute Pericarditis
What is Acute Pericarditis: Signs and Signals
Addressing Recurrent Pericarditis
Guidelines and Articles
- 2014 AHA/ACC Guideline for the Management of Patients With Non-ST-Elevation Acute Coronary Syndromes (PDF)
- Cardiovascular Disease and Breast Cancer: Where These Entities Intersect: A Scientific Statement From the American Heart Association. Circulation. 2018;137:e30–e66.
- ACC/AHA/ESC 2006 Guidelines for the Management of Patients with Atrial Fibrillation - Full Text. Circulation. 2006;114:e257–e354.